
Made possible through support from The DentaQuest Foundation.
FACT SHEET | UPDATED SEPTEMBER 2019
Medicaid Adult Dental Benefits: An Overview
ow-income adults suffer a disproportionate share of dental disease, and are nearly
40 percent less likely to have a dental visit in the past 12 months, compared to those
with higher-incomes.
1
Forty-four percent of low-income adults ages 20 to 64 have
untreated tooth decay, and five percent of adults have lost all of their teeth.
2
Adults who are
disabled, homebound, or institutionalized have an even greater risk of dental disease.
3
Poor oral health can elevate risks for chronic conditions such as diabetes and heart disease,
as well as for lost workdays and reduced employability.
4
It can also lead to the preventable
use of costly acute care. A recent study identified $2.7 billion in dental-related hospital
emergency department visits in the U.S. over a three-year period. Thirty percent of these
visits were by Medicaid-enrolled adults, and over 40 percent were by uninsured individuals.
5
Challenges to Oral Health Care Access and Utilization
for Low-Income Adults
Inadequate Dental Coverage: While comprehensive dental coverage is mandatory for children enrolled in Medicaid, dental
benefits for Medicaid-eligible adults are optional. States have considerable flexibility in determining the scope of dental services
covered. As a result, Medicaid adult dental coverage varies tremendously across states, and is limited in some cases to
emergency services such as tooth extractions, or to specific populations such as pregnant women.
6
In response to fiscal
challenges in the early 2000s, many states reduced or eliminated Medicaid dental coverage over the course of a decade,
7
with
a concurrent 10 percent decline in oral health care utilization among low-income adults.
8
A small increase in utilization rates
has since been observed among adults with public insurance and may be due in part to Medicaid expansion under the
Affordable Care Act.
9
Insufficient Provider Availability: Medicaid enrollees often have difficulty finding Medicaid-contracted dental providers.
Only 39 percent of dentists nationwide accept Medicaid and/or the Children’s Health Insurance Plance (CHIP), citing
burdensome administrative requirements, missed appointments, lengthy payment wait times, and low reimbursement rates as
barriers to participation.
10, 11
Individual Barriers: Disparities in dental access and utilization for low-income adults are often exacerbated by challenges in
making work or child care arrangements and/or obtaining transportation to appointments as well as covering the cost of
required copayments. Additional issues that may pose barriers include: (1) a lack of awareness of dental benefits; (2) gaps in
oral health literacy; (3) the perception that oral health is secondary to general health; and (4) primary care providers who may
not encourage oral health care.
12, 13
Medicaid Coverage of Adult Dental Benefits: Medicaid Base and Expansion Populations
The ACA provided new opportunities for states to leverage federal dollars and extend dental access to low-income adults
through Medicaid expansion. A state can offer a dental benefits package to its expansion population that is either the same or
different than what is provided to its base Medicaid population.
14
Dental benefits covered by state Medicaid programs typically
fall into three general categories:
15
Emergency Only: Relief of pain under defined emergency situations.
Limited: Fewer than 100 diagnostic, preventive, and minor restorative procedures recognized by the American Dental
Association (ADA); per-person annual expenditure for care is $1,000 or less.
Extensive: A comprehensive mix of services, including more than 100 diagnostic, preventive, and minor and major
restorative procedures approved by the ADA; per-person annual expenditure cap is at least $1,000.
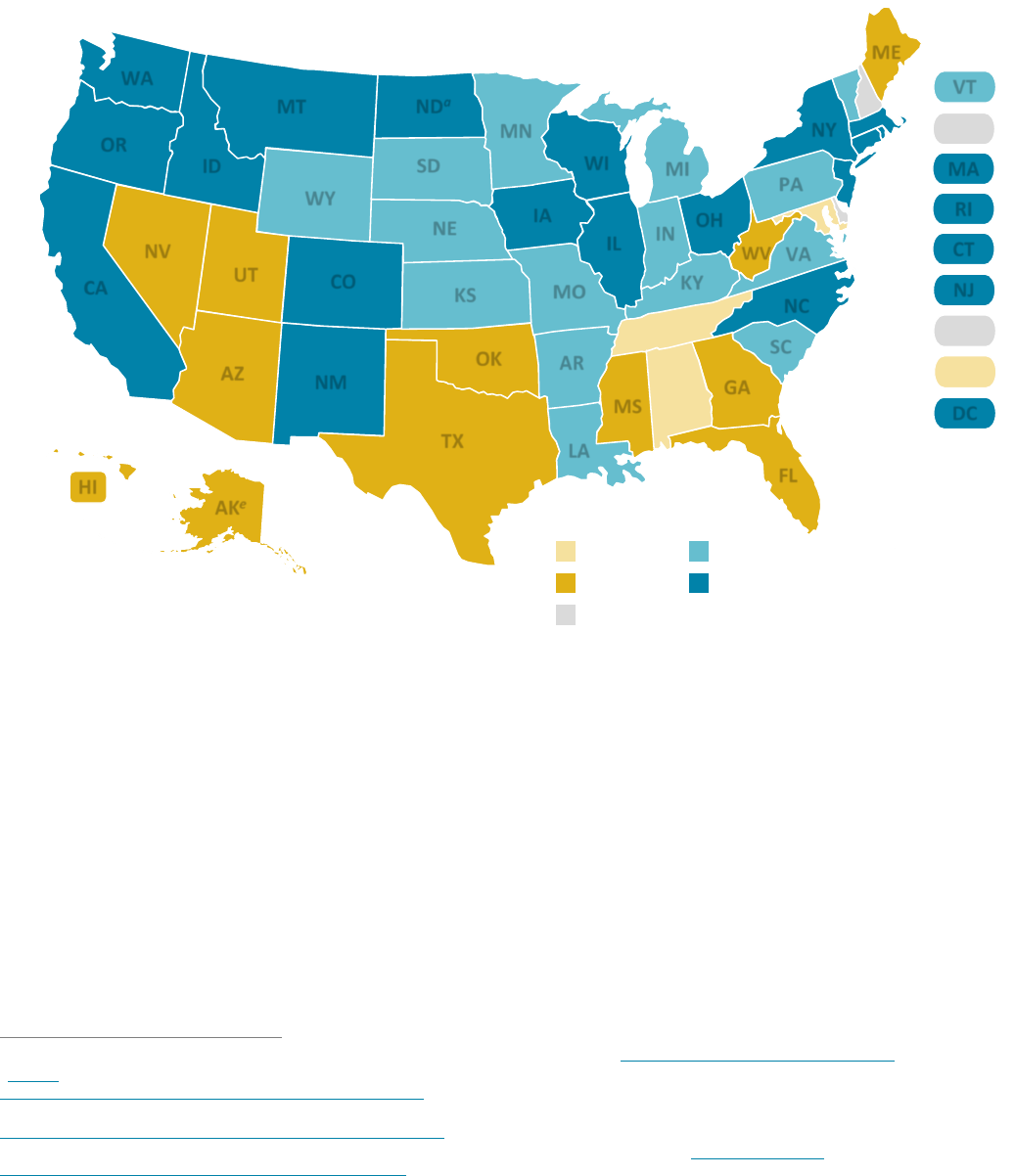
Nearly all states (47) and D.C. offer some dental benefit to their base adult Medicaid population (see Exhibit 1, next page).
Thirty-six (including D.C.) cover services beyond defined emergency situations (e.g., uncontrolled bleeding, traumatic injury),
and among those, 19 (including D.C.) cover extensive services. All but one of the states currently expanding Medicaid — North
Dakota — offer the same dental benefits package to both their base and expansion populations.
L
FACT SHEET | Medicaid Adult Dental Benefits: An Overview
Advancing innovations in health care delivery for low-income Americans | www.chcs.org
EXHIBIT 1. State Medicaid Coverage of Adult Dental Benefits, September 2019
a
b
Under New Hapshire’s bill the Department of Health and Human Services is directed to develop a “comprehensive plan to ensure that Medicaid recipients can
safeguard their smiles and their overall health.”
c
Under Delaware’s bill the state will offer preventive and restorative dental coverage to adult Medicaid beneficiaries.
d
Maryland offers treatment for symptoms in emergency situations but does not cover emergency surgery.
e
Alaska’s state budget was passed keeping adult dental coverage intact; however, the Governor’s line item vetoes in the budget will result in cuts to the state’s
Medicaid program, including adult dental, unless the legislature moves to rescind them.
State Strategies to Increase Dental Coverage and Access for Adults
States are engaging in a variety of strategies to promote adult coverage and access to oral health care. These include tailoring
oral health literacy campaigns to educate eligible adults about coverage options; developing coalitions of likeminded partners
to build political support; and expanding the dental workforce to include mid-level providers such as dental therapists, who can
be trained and licensed to perform preventive care and routine restorative procedures.
16
States are additionally targeting
coverage for vulnerable adult populations within Medicaid, including pregnant women, individuals with diabetes, and adults
with disabilities.
17
1
Centers for Disease Control and Prevention. “Oral and Dental Health: Table 78.” May 2017. Available at: https://www.cdc.gov/nchs/fastats/dental.htm.
2
National Institute of Dental and Craniofacial Research. “Dental Caries (Tooth Decay) in Adults (Age 20 to 64).” July 2018. Available at:
https://www.nidcr.nih.gov/research/data-statistics/dental-caries/adults.
3
The Institute of Medicine. “Improving Access to Oral Health Care for Vulnerable and Underserved Populations.” 2011. Available at:
http: //www.hrsa.gov/publichealth/clinical/oralhealth/improvingaccess.pdf
.
4
National Academy for State Health Policy. “Medicaid Coverage of Adult Dental Services.” October 2008. Available at https://nashp.org/wp-
content/uploads/sites/default/files/Adult%20Dental%20Monitor.pdf.
5
V. Allareddy, S. Rampa, M. Lee, V. Allareddy, and R. Nalliah. “Hospital-based Emergency Department Visits Involving Dental Conditions: Profile and Predictors of
Poor Outcomes and Resource Utilization. Journal of the American Dental Association, 145, no.4 (2014): 331-337.
WY
WI
WV
WA
VA
VT
UT
TX
TN
SD
SC
RI
PA
OR
OK
OH
ND
a
NC
NY
NM
NJ
NH
b
NV
NE
MT
MO
MS
MN
MI
MA
MD
d
ME
LA
KY
KS
IA
IN
IL
ID
HI
GA
FL
DC
DE
c
CT
CO
CA
AR
AZ
AK
e
AL
No coverage
Limited
Emergency
-only
Extensive
Under
development
KEY

FACT SHEET| Medicaid Adult Dental Benefits: An Overview
Advancing innovations in health care delivery for low-income Americans | www.chcs.org
6
C. Yarbrough, M. Vujicic, and K. Nasseh. More than 8 Million Adults Could Gain Dental Benefits through Medicaid Expansion. Health Policy Institute, American
Dental Association, February 2014. Available at http://www.ada.org/~/media/ADA/Science%20and%20Research/HPI/Files/HPIBrief_0214_1.ashx
.
7
National Conference of State Legislatures. “Health Cost Containment and Efficiencies: NCSL Briefs for State Legislators.” 2014. Available at:
http://www.ncsl.org/documents/health/IntroandBriefsCC-16.pdf
.
8
Note: This decline was from 2002-2010. M. Vujicic. Dental Care Utilization Declined among Low-income Adults, Increased among Low-Income Children in Most
States from 2000 to 2010. Health Policy Institute, American Dental Association, February 2013. Available at
http://www.ada.org/~/media/ADA/Science%20and%20Research/HPI/Files/HPIBrief_0213_3.ashx
.
9
K. Nasseh and M. Vujicic. Dental Care Utilization Steady Among Working-Age Adults and Children, Up Slightly Among the Elderly. Health Policy Institute,
American Dental Association, October 2016. Available at: http://www.ada.org/~/media/ADA/Science%20and%20Research/HPI/Files/HPIBrief_1016_1.pdf
.
10
Subcommittee on Primary Health and Aging. “Dental Crisis in America: The Need to Expand Access.” U.S. Senate Committee on Health, Education Labor and
Pensions, February 2012. Available at: http://www.sanders.senate.gov/imo/media/doc/DENTALCRISIS.REPORT.pdf
.
11
Health Policy Institute and American Dental Association. “Dentist Profile Snapshot by State 2016.” January 2018. Available at: https://www.ada.org/en/science-
research/health-policy-institute/data-center/supply-and-profile-of-dentists.
12
The Kaiser Commission on Medicaid and the Uninsured, op cit.
13
Ibid.
14
S. Chazin, V. Guerra, and S. McMahon. Strategies to Improve Dental Benefits for the Medicaid Expansion Population. Center for Health Care Strategies, February
2014. Available at http://www.chcs.org/media/CHCS-Revised-Adult-Dental-Benefits-Brief__021214.pdf
.
15
Ibid.
16
Ibid.
17
C. Le and M. Burroughs. Oral Health Coverage in the 2019 State Legislatures: Victories, Budget Cuts, and Opportunities for Future Progress. Families USA, July
2019. Available at: https://familiesusa.org/sites/default/files/product_documents/OH_2019-Legislative%20WrapUp_Anaylsis.pdf
.
