
ISSUE BRIEF
Medicaid Waivers:
A Vehicle to Improve Access
to Oral Health & Address
Disparities for Older Adults
and People with Disabilities
MAY 2024
Amber Christ, Managing Director, Health Advocacy
Samantha Morales, Senior Policy Advocate
INTRODUCTION
Access to oral health care is essential to the overall health of older adults and people with disabilities and to
addressing health disparities. Unfortunately, however, oral health coverage for these populations is limited.
Traditional Medicare—the primary health insurance program for older adults and people with disabilities—does
not include an oral health benet. For those enrolled in private Medicare plans known as Medicare Advantage or
in standalone dental plans, coverage is varied and can include signicant out-of-pocket costs.
By default, Medicaid is the primary source of oral health coverage for low-income older adults and people with
disabilities. However, under federal law, states are not required to oer adult dental coverage in their Medicaid
programs. As a result, Medicaid oral health coverage varies from state to state. is is particularly problematic
for older adults and people with disabilities, who, because of age and disability, are more likely to have poor
oral health and also more likely to have chronic conditions that are exacerbated by poor oral health. Even if
dental treatment is covered under Medicaid, older adults and people with disabilities can face unique barriers to
actually accessing the care they need.
Enter Medicaid waivers, which allow states to “waive” certain requirements under federal law in order to more
exibly design their Medicaid programs to meet the needs of enrollees. For oral health, waivers can serve as an
important tool for states to both expand the extent of oral health coverage available and as a means of addressing
the unique barriers older adults and people with disabilities face in accessing covered dental treatment.
is issue brief is intended to equip state oral health, aging, and disability advocates with education and
advocacy tips on how to leverage Medicaid waivers to expand access to oral health and address disparities in
access to dental treatment. e issue brief begins with an explanation of Medicaid waivers, including what they
do and who they impact. is is followed by state-specic examples illustrating how Medicaid waivers can
both expand the scope of coverage available and address barriers to care. e brief concludes with steps on how
advocates can engage in the waiver process.

JUSTICE IN AGING | ISSUE BRIEF | www.justiceinaging.org | 2
MEDICAID ADULT DENTAL COVERAGE BY STATE
States are not required to offer adult dental benets in their Medicaid programs. As a result, whether a state
offers dental coverage, to what extent, and to what populations vary signicantly from state to state.
1
The CareQuest Institute maintains a Medicaid Adult Dental Coverage Tracker that advocates can review to
determine the status of Medicaid coverage in their state.
2
The tracker demonstrates that advocates have
made enormous progress in expanding adult dental coverage, but signicant coverage gaps persist.
MEDICAID WAIVERS: AN OVERVIEW
Under federal law, states are required to cover certain populations and benets in their Medicaid programs.
3
States also can cover other benets and populations at their option. For example, states are mandated to cover
hospital services, physician services, and care in a nursing facility, whereas states have the option to cover
dental, vision, hearing, and at-home care. States must outline what populations and benets they will cover in a
document called the Medicaid State Plan, which is a formal agreement between the state and federal government
approved by the Centers for Medicare & Medicaid Services (CMS).
4
From nearly the outset of the Medicaid program, Congress recognized that states needed exibility in designing
their Medicaid programs to go beyond their State Plan agreements in order to eectively serve their populations.
is exibility is granted through Medicaid waiver authority, which, if approved by CMS, permits states to
disregard certain federal requirements that are otherwise binding on Medicaid programs. Such exibility includes,
for example, allowing states to target programs and benets to specic populations and test innovative ways of
delivering care. is paper focuses on three types of Medicaid waivers: Medicaid Home and Community-Based
Services (HCBS) waivers, also known as 1915(c) waivers, 1115 demonstration waivers; and 1915(b) Medicaid
Managed Care waivers.
5
Medicaid 1915(c) HCBS Waivers
Medicaid Home and Community-Based Services (HCBS) refers to a broad set of long-term health and social
services and supports provided to an individual in their own home and integrated community-based settings, as
opposed to institutional settings such as a nursing facility.
6
Like adult dental coverage, states are not required to
cover HCBS in their Medicaid programs. However, unlike adult dental, all states do cover HCBS.
e 1915(c) waiver authority is one means a state can use to oer HCBS to their Medicaid populations. In
order to be eligible for 1915(c) waiver programs, individuals must have signicant healthcare needs and require
assistance with daily activities at a nursing facility level of care. In other words, but for the availability of the
1915(c) covered benets, the individual would qualify for Medicaid coverage in a nursing facility.
Common 1915(c) waiver programs serve specic populations including, for example, older adults with Alzheimer’s
and dementia, people with developmental disabilities of all ages, adults with physical disabilities, and people with
traumatic brain injury. Benets under these waivers include personal care services such as providing help with
bathing, dressing, and eating; homemaker and chore services; home modications; adult day services; assisted
living; durable medical equipment; caregiver respite; and care management.
As of 2024, all states except for Arizona, New Jersey, Rhode Island, and Vermont, operated one or more 1915(c)
waiver programs for one or more specic populations.
7

JUSTICE IN AGING | ISSUE BRIEF | www.justiceinaging.org | 3
1115 Demonstration Waivers
e 1115 demonstration waiver allows states to test new approaches to delivering care to their Medicaid
populations. States use 1115 waiver authority to implement creative and expansive changes in their Medicaid
programs, including changes to eligibility, benets, and how care is delivered. For example, states have used 1115
waivers to change the delivery of care from fee-for-service to requiring their Medicaid populations receive their
care through a health plan (managed care); to expand and target benets for focus populations, like those leaving
incarceration or individuals experiencing homelessness; and to increase nancial eligibility criteria for targeted
populations. While 1915(c) waivers are narrow, applying only to HCBS benets for people with disabilities, 1115
waivers can be very broad and aect nearly any aspect of a Medicaid program.
1915(b) Waivers
e 1915(b) waiver is specic to managed care and permits states to waive freedom of choice and require its
Medicaid populations to enroll in a health plan. States also use the 1915(b) waiver to oer specic benets only to
managed care enrollees and to limit the providers the state contracts with to deliver specic benets.
USING MEDICAID WAIVERS TO EXPAND ACCESS TO
ORAL HEALTH AND ADDRESS DISPARITIES
Medicaid waivers can be a powerful vehicle for expanding access to oral health for older adults and people with
disabilities in all states regardless of the current status of coverage. For example, in states with minimal adult
dental coverage, Medicaid waivers can be used to expand coverage specically to older adults and people with
disabilities when state advocacy to obtain a more comprehensive dental benet for all adults is ongoing or stalled.
At the same time, Medicaid waivers can provide additional services and supports to address specic barriers to
covered dental treatment and help reduce the disparities in access and quality of care older adults and people with
disabilities face.
State advocates are best positioned to utilize Medicaid waivers to expand oral health in a way that is responsive
to the needs of residents in their state and that accounts for their state’s dynamic budget and political reality. e
examples oered below are not exhaustive but are meant to illustrate ways in which waivers can be utilized in
states with very dierent Medicaid coverage, budget, and political landscapes to better meet the oral health needs
of older adults and adults with disabilities. e Appendix provides a comprehensive overview of existing waivers
by state that include oral health benets.
DISPARITIES IN ACCESS TO ORAL HEALTH CARE
Even when older adults and people with disabilities have access to oral health coverage, they face unique
barriers obtaining the care they need, leading to disparities in access and health outcomes. For example,
individuals with cognitive impairments may require additional time with an oral health provider to receive
adequate treatment or require sedation; people who cannot easily leave their homes may need access to
mobile units or teledentistry; people with physical disabilities may require someone to perform oral hygiene or
need modied oral hygiene products. These barriers are compounded by existing discrimination and barriers
in the health care system based on race, ethnicity, language, sexual orientation, and gender identity, and
where someone lives—e.g. rural versus urban or at home or in an institutional setting. For additional resources
on addressing disparities, see Justice in Aging’s Adding a Dental Benet to Medicare: Addressing Racial
Disparities and Adding a Dental Benets to Medicare: Addressing Oral Health Inequity Based on Disability.

JUSTICE IN AGING | ISSUE BRIEF | www.justiceinaging.org | 4
Using Waivers to Expand Dental Coverage in States with Minimal
Adult Coverage
For states that have minimal to no adult dental coverage under their State Plan, Medicaid waivers can provide
more extensive coverage to targeted populations with specic health care needs. is use of a Medicaid waiver can
provide oral health coverage to people with the most complex health care needs while also building evidence to
support the expansion of coverage to all adults in the state. Put another way, waivers can be a building block or
step in obtaining extensive adult dental coverage in the state.
Kansas as a Case Study
Prior to 2022, Kansas provided limited adult dental coverage—adults were generally entitled to emergency
dental care only. From 2008 to 2010, however, the state provided comprehensive dental coverage for people
enrolled in the HCBS Frail Elderly, Physical Disabilities, and Intellectual and Developmental Disabilities waivers.
The funding for dental coverage in these waivers was cut during the Great Recession, and Medicaid coverage
reverted to emergency dental care only for all populations.
Over the next decade, oral health, disability, and aging services advocates worked together to uplift the
positive experience of having dental coverage in the HCBS waivers for older adults and people with disabilities
to advocate for coverage for all adults enrolled in Medicaid. Advocates cited the successes of offering dental
coverage to the more limited population to make the case that extending coverage to all adults would similarly
improve health outcomes and generate savings, as well as be more fair and equitable than only offering
coverage to a limited subset of the state’s Medicaid population.
8
In 2022, Kansas advocates were successful in extending adult dental benets under the Medicaid state plan
for all adults including coverage for periodontal care, silver diamine uoride treatments, llings, and crowns.
Denture coverage was added in 2023, and the Kansas Legislature approved funding for preventive dental care
for adults in 2024.
9
Using Waivers to Expand Coverage Beyond State Plan Benets
Some states oer adult dental benets, but there are gaps in coverage. For example, a state may oer preventive
services and some restorative care, like root canals, but not oer periodontal treatment (gum treatment) to all
or a subset of its Medicaid population. Below are examples of how states are using Medicaid waivers to expand
coverage beyond state plan benets to targeted populations.
South Carolina Community Choices
The South Carolina Community Choices 1915(c) waiver serves individuals 65 and over who are dually eligible for
Medicare and Medicaid with a nursing home level of care need and individuals with physical disabilities ages
18 to 64. As part of this waiver, the state covers dentures as a one-time expense not to exceed $651.00 per
plate or $1,320.00 for one full pair of dentures. The state will also cover denture repair not to exceed $77.00 per
occurrence.
10
Dentures are not available to adults outside of the state’s 1915(c) waiver.
Florida Familial Dysautonomia 1915(c) Waiver
Florida provides HCBS through a 1915(c) waiver to eligible enrollees diagnosed with Familial Dysautonomia,
a rare genetic disorder affecting nerves that control breathing and digestion. Enrollees in the Florida Familial
Dysautonomia Waiver between the ages of 3 to 64 who require a hospital level of care can receive adult dental
services not otherwise covered by the Medicaid State Plan including diagnostic, preventive, and restorative
treatment, and endodontics, periodontal, and surgical procedures.
11

JUSTICE IN AGING | ISSUE BRIEF | www.justiceinaging.org | 5
California Advancing and Innovating Medi-Cal (CalAIM) 1115 Waiver
California uses its CalAIM 1115 waiver to cover Silver Diamine Fluoride (SDF) treatment, which is currently not
covered under the Medicaid State Plan. SDF is used to prevent tooth cavities from forming and spreading. The
waiver allows for SDF treatment to be administered to children (ages 0-6) and, importantly for this issue brief,
to persons with underlying conditions that make it unlikely that nonrestorative treatment will be successful,
including residents in skilled nursing facilities and individuals with intellectual and developmental disabilities.
12
Using Waivers to Address Barriers to Treatment
Older adults, people with disabilities, and members of marginalized communities who have oral health coverage
still face challenges in accessing oral health treatment. Such challenges include, for example, a dental oce
being dicult to travel to or physically inaccessible; needing extra time for dental treatment to be rendered; and
requiring assistance with oral hygiene. Below are examples of states using Medicaid waivers to help address these
barriers to treatment and disparities in access.
Michigan Health Link 1915(c) HCBS Waiver
The MI Health Link Waiver program offers HCBS through managed care to individuals dually eligible for
Medicare and Medicaid. Through this waiver, enrollees are eligible to receive devices and appliances to help
them perform their activities of daily living, including modied oral hygiene aids like toothbrush adaptors and
oral swabs, free of charge.
13
Mississippi Independent Living 1915(c) Waiver
As part of Mississippi’s Independent Living 1915(c) waiver that serves individuals over the age of 65 and
individuals between 0 to 64 years old living with physical and other disabilities, personal care attendants are
required to be trained on oral hygiene.
14
Utah Choice of Dental Care Delivery Program
Under Utah’s 1915(b) managed care waiver, the state requires contracted dental plans to ensure the delivery
of dental benets to specic populations, including children with disabilities, through targeted strategies.
15
Specically, the state requires contracted dental plans to ensure direct access to specialists, that each enrollee
has an ongoing source of primary dental care, and to use independent monitors to analyze demographic data to
assess access and health disparities.
HOW TO ADVOCATE FOR ORAL HEALTH COVERAGE IN
HCBS WAIVERS
Center Equity
e ways Medicaid waivers can be used to expand coverage and improve access to care are innite. In advocating
for oral health expansions and improvements through Medicaid waivers, advocates should consider policies
that would address the disparities that older adults, people with disabilities, and members of marginalized
communities face in accessing oral health care. Coverage is an essential piece of access but alone cannot
address disparities.
At a minimum, every HCBS waiver should explicitly require personal care attendants to be trained to perform
oral hygiene, similar to what federal law requires for nurse aids in nursing facilities. Waivers could also make
JUSTICE IN AGING | ISSUE BRIEF | www.justiceinaging.org | 6
oral health care accessible through co-location with medical care, like allowing doctors to apply uoride varnish,
through teledentistry, and by facilitating quick compliance with requirements to have accessible exam chairs.
16
Waivers could require training that is culturally competent and tailored for people with specic disabilities and
health care conditions, improve access to sedation through higher reimbursement rates, and allow additional
reimbursed time for rendering oral health services. ese are just a few examples of policies that could help
address disparities in oral health access and outcomes based on age, disability, race, and other factors.
Comment on Waiver Applications
States are required to seek public input in the development and approval of waivers. Advocates can use the public
commenting opportunity to advance proposals to include in waivers that improve oral health.
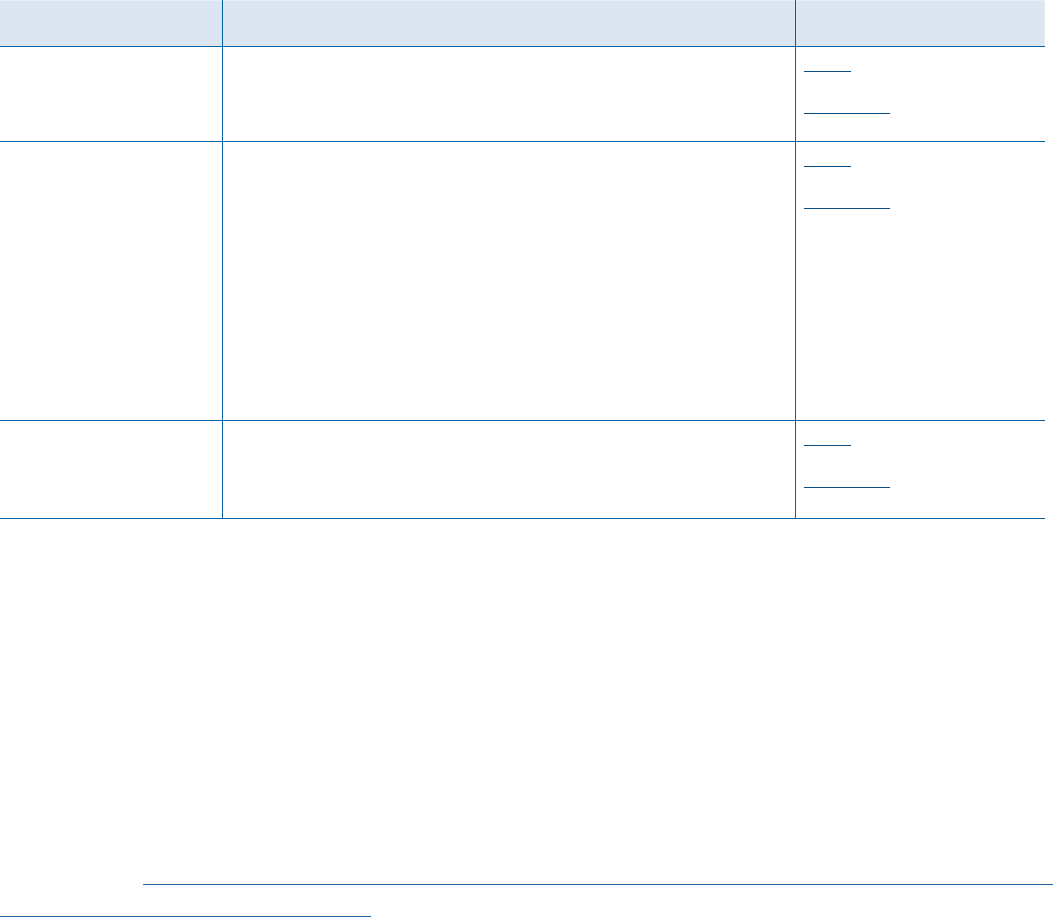
Waiver Comment Process and Timelines
MEDICAID WAIVER COMMENT PROCESS APPROVAL PERIODS
1915(c)
17
States are required to provide at least a 30-day notice and
comment period prior to submission of the waiver application
to CMS.
Initial: 3 years
Extension: up to 5 years
1115
18
States are required to provide at least a 30-day public notice
and comment period for applications for both new 1115
demonstrations and for extensions and amendments to
existing demonstrations.
States also must conduct at least two public hearings on
separate dates and at separate locations and accept public
comment.
After the application is submitted to CMS, CMS provides a
second 30-day comment period.
Initial: 5 years
Extension: 3-5 years
1915(b)
19
States are required to provide at least a 30-day notice and
comment period prior to submission of the waiver application
to CMS.
Initial: 2 years
Extension: 2 years
CONCLUSION
Medicaid waivers are an invaluable tool for addressing the signicant disparities in access to dental treatment
faced by older adults and people with disabilities. It is imperative that aging, disability, and oral health advocates
and providers engage in public comment opportunities to advocate for the inclusion of oral health in Medicaid
waivers. By harnessing the potential of Medicaid waivers, we can move closer towards ensuring that all
individuals have access to the oral health care they need to thrive.
APPENDIX
e Appendix, Medicaid Waivers with Oral Health Benets for Older Adults and Adults with Disabilities by State, is
available on the Justice in Aging website.

JUSTICE IN AGING | ISSUE BRIEF | www.justiceinaging.org | 7
ENDNOTES
1 National Academy for State Health Policy (NASHP), State Medicaid Coverage of Dental Services for General Adult and
Pregnant Populations, (updated Oct. 20, 2022). See also, Medicaid and CHIP Payment and Access Commission (MACPAC),
Access to Covered Dental Benets for Adult Medicaid Beneciaries: Panel Discussion (Apr. 13, 2023).
2 CareQuest Institute for Oral Health, Medicaid Adult Dental Tracker, last accessed May 8, 2024.
3 Medicaid.gov, Mandatory & Optional Medicaid Benets, last accessed May 8, 2024.
4 MACPAC, State Plan, last accessed May 8, 2024. Adult dental benets are located in Section 3 of the State Plan.
5 Medicaid waivers are named after the statutory section of the Social Security Act in which they are found, Social Security Act, 42
U.S.C. §§ 1915(b); 1915(c); and 1115.
6 Justice in Aging, Medicaid Home- and Community-Based Services for Older Adults with Disabilities: A Primer (Apr. 2021).
7 Medicaid.gov, State Waivers List, last accessed May 8, 2024.
8 e authors would like to thank Tanya Dorf Brunner, Executive Director of Oral Health Kansas for contributing to this paper.
9 Kansas Dept. of Health and Environment, Update for Dental Coverage for Ages 21 and Over (Jun. 2022); Coverage of Denture
and Partial Prosthetics for Ages 21 and Older (Jun. 2023); Oral Health Kansas, Weekly Wednesday Update (May 1, 2024).
10 Medicaid.gov, SC Community Choices Waiver, (0405.R04.00), last accessed May 8, 2024.
11 Medicaid.gov, FL Familial Dysautonomia Waiver, (40205.R03.00), last accessed May 8, 2024.
12 California Department of Health Care Services, Silver Diamine Fluoride, last accessed May 8, 2024.
13 Medicaid.gov, MI Health Link HCBS Waiver, (1126.R01.00), last accessed May 8, 2024.
14 Medicaid.gov, MS Independent Living Waiver (0255.R07.00), last accessed May 8, 2024.
15 Medicaid.gov, Choice of Dental Care Delivery Program, (UT-0004), last accessed May 8, 2024.
16 45 CFR § 84.90 et seq.
17 CMS, Application for a §1915(c) Home and Community-Based Waiver: Instructions, Technical Guide and Review Criteria,
(Jan. 2019).
18 42 CFR Part 431
19 MACPAC, 1915(b) Wa ivers, last accessed May 8, 2024.
